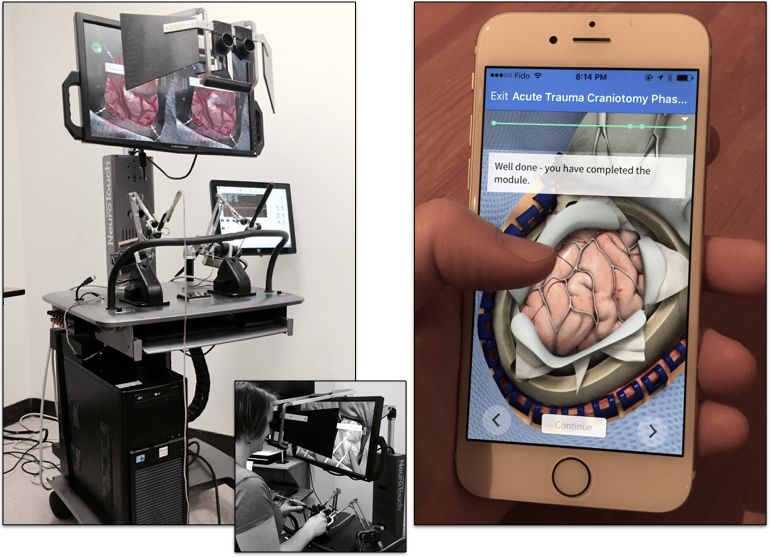
by Marta Kersten-Oertel
About eight years ago, Canada’s National Research Council (NRC) teamed with a number of Canadian teaching hospitals to develop NeuroTouch, a neurosurgical simulator. The goal of this collaborative effort was to improve resident training by creating an environment where trainees could practice procedures and develop skills prior to entering the operating room. In the aviation industry, pilots learn some of the most difficult aspects of flying in flight simulators. They are required, as part of their training, to record hundreds of hours in simulators prior to flying an actual plane. Looking towards aviation as an example, the aim of the project was to go beyond the learning methodology of ‘see one, do one, teach one’ and offer a training environment that would develop skills as well as minimize adverse events in real-life surgical cases.
Although studies have shown that certain technical skills can be learned using the NeuroTouch and that it can provide performance benchmarks, it is hard to conclude that surgeries performed by residents or junior surgeons who train using such simulators are less prone to adverse events. The fact that the use of these simulators has been limited to a few academic centers is likely the result not only of their cost but also due to a lack of large studies validating the effectiveness of this type of training. Perhaps, with CAE’s (a world industrial leader in simulation technology) recent acquisition of the exclusive rights of the NeuroTouch (now NeuroVR) there is greater potential for integration of these systems into medical training programs.
In comparison to these expensive realistic surgical simulators, over the last couple of years, apps that offer simple simulations have been developed to provide a way to ‘e-learn’ surgeries. According to Andre Chow, surgeon and co-founder of Touch Surgery, unlike realistic surgical simulators that focus on teaching technical skills (which account for 25% of a safe operation), the goal of such apps is to teach the steps and key decision points during surgery (which account for 75% of a safe operation). These simple apps allow trainees and OR staff to brush-up on the key components of a particular surgery anywhere and anytime. To study this Conquer Mobile has recently teamed up with Dalhousie University (Halifax, N.S.) to look at how their PeriopSim app can be used by nurses to refresh their knowledge of surgical instruments for specific surgical steps.
Is there a place and use for simple free or low-cost apps and high-fidelity expensive simulators? Only time will tell but certainly one can envision a student building their experiences on simple apps while perfecting the technical skills on more realistic simulators. Over the next few years, we should see more research done on the impact of these technologies on trainees and practitioners. The combination of commercial investment into a high-end surgical simulator and the development of simple surgical workflow apps might just be the push needed to bring simulation from more research-intensive environments to everyday use in medical training.

Leave a Reply